What is the Average Allowed Amount for Behavioral Health in California with Anthem Blue Cross?
Price for Behavioral Health Care with Anthem
For healthcare providers, one of the most persistent challenges is determining if they are being paid a fair rate. Understanding how your reimbursements compare to the rest of the market is essential for contract negotiations and financial planning.
The CMS Price Transparency mandate now allows providers to look directly at the negotiated rates between payers and facilities. By accessing these machine-readable files, we can analyze the “allowed amounts”—the maximum amount a plan will pay for a covered health care service.
Benchmarking Anthem Blue Cross California Rates
To provide a clear picture of the current landscape, we filtered the latest transparency data for Anthem Blue Cross California specifically for Behavioral Health CPT codes.
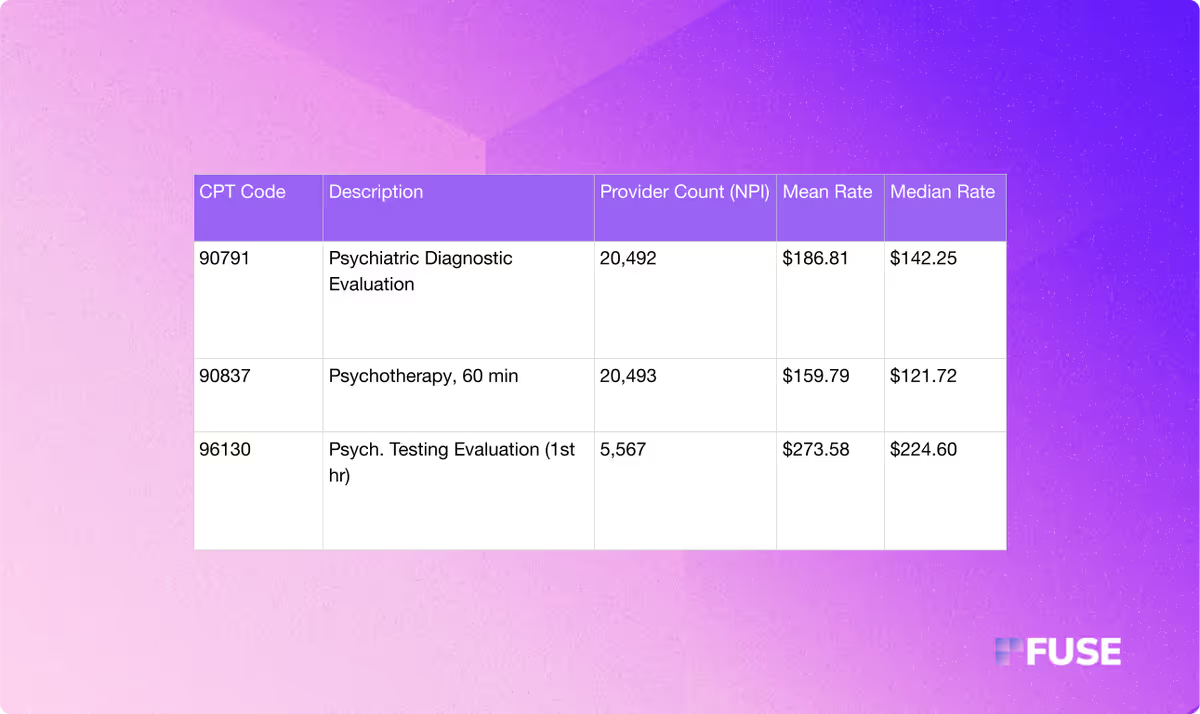
Below are the negotiated rate results for key CPT codes:
-
CPT 90791 (Psychiatric Diagnostic Evaluation)
- Unique NPI Count: 20,492
- Mean Negotiated Rate: $186.81
- Median Negotiated Rate: $142.25
-
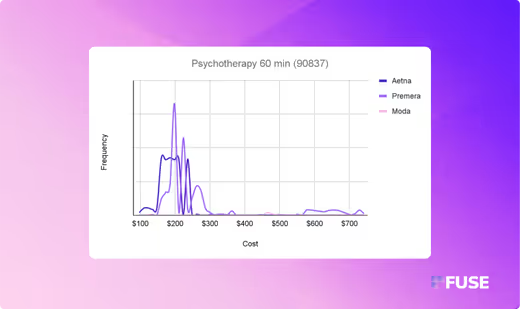
CPT 90837 (Psychotherapy, 60 minutes)
- Unique NPI Count: 20,493
- Mean Negotiated Rate: $159.79
- Median Negotiated Rate: $121.72
-
CPT 96130 (Psychological Testing Evaluation, 1st hour)
- Unique NPI Count: 5,567
- Mean Negotiated Rate: $273.58
- Median Negotiated Rate: $224.60
Key Insights from the Data
The data reveals the following benchmarks for Anthem’s behavioral health network in California:
- 90791 (Diagnostic Evaluation): The median rate for an initial evaluation sits at $142.25. The significantly higher mean of $186.81 indicates that a portion of the 20,000+ providers in this network have negotiated rates well above the midpoint.
- 90837 (60-Minute Psychotherapy): As one of the most frequently billed codes, the median negotiated rate is $121.72.
- 96130 (Testing Evaluation): This specialized service commands the highest reimbursement in this set, with a median rate of $224.60.
Disclaimer: The data provided is based on publicly available CMS machine-readable files and represents a snapshot of negotiated rates. Individual reimbursements may vary based on provider credentials, specific contract terms, and facility type.