Streamline Your Revenue Cycle with Frontend Healthcare Automation
Manual revenue cycle processes slow everything down before a claim is ever submitted. Incomplete patient intake, missing insurance details, and rushed eligibility checks create bottlenecks that ripple from registration through billing and payment. By the time denials appear, the real problem has already happened upstream.
Fuse focuses on automating the front end of the revenue cycle, where most preventable issues start. We automate patient intake, insurance verification at the CPT code level, payer portal checks, direct payer calls, and fee estimates so your team doesn't have to. The result is fewer downstream problems and more time for staff to focus on patients instead of administrative work.







Patient Trust
Streamlined RCM for eligibility and benefits checks leads to accurate patient cost estimates, better collections and an improved experience. Offer price transparency and reduce overhead with automation powered by Fuse.
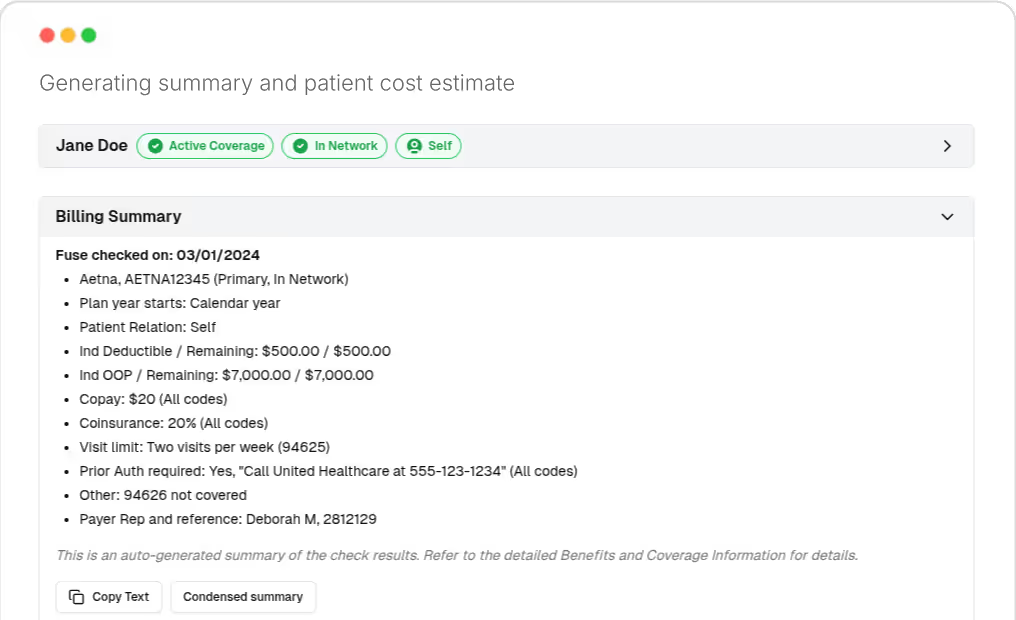

Accurate Fee Estimates From Granular Benefits Data
Accurate pricing starts with accurate benefits data. Fuse uses granular payer information to generate upfront patient cost estimates tied to specific CPT codes. Instead of vague ranges, patients see a clear breakdown of deductibles, copays, and coinsurance.
This transparency improves the patient experience and makes financial conversations easier for staff. Practices that provide clear estimates upfront see fewer billing disputes and stronger collections, especially for higher-cost services.

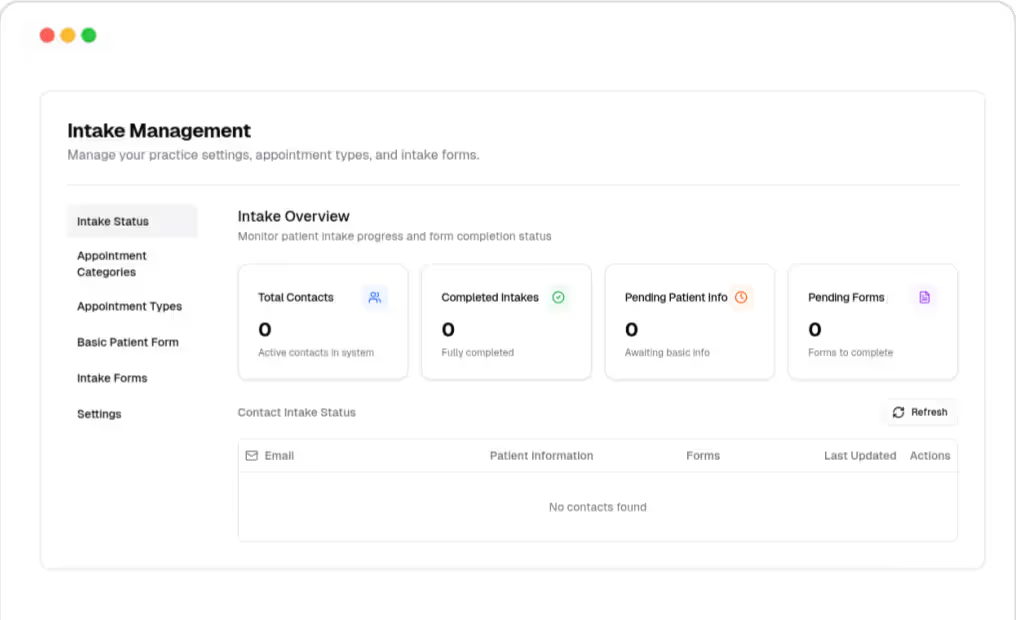
Our Patient Intake Integrates With Insurance Checks
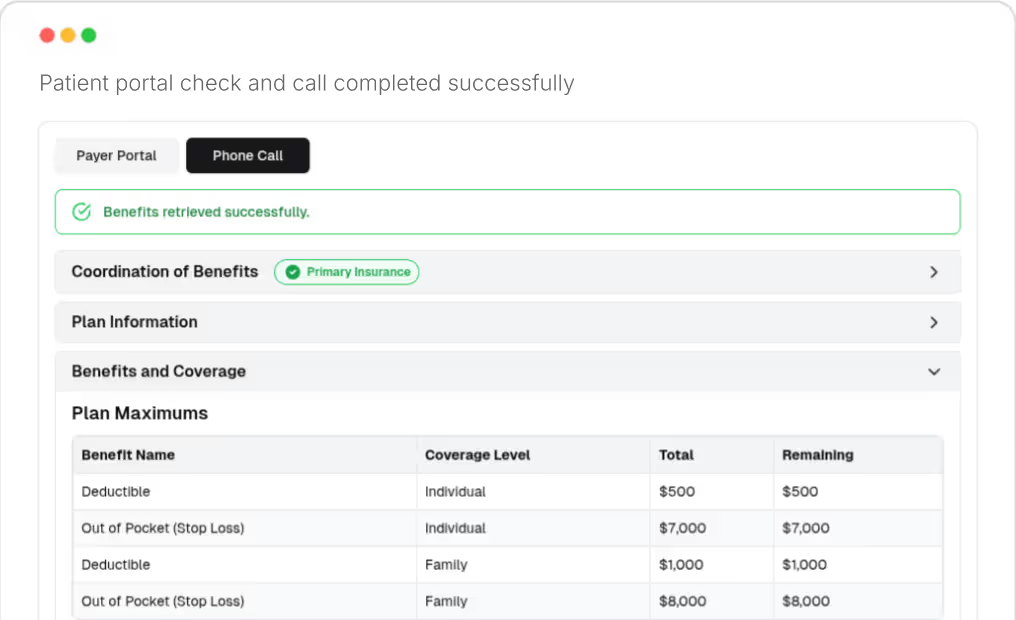
Fuse's biggest advantage is how intake and insurance verification work together. Patients upload their insurance details directly into Fuse, removing the need for staff to chase cards or re-enter data. Fuse verifies that information, checks coverage, and returns CPT-level benefits with a clear summary of both portal and phone call results.
This end-to-end process is extremely time-consuming for most clinics when done manually. Fuse integrates it into one connected workflow. Intake is also available at no cost to clinics using Fuse's insurance verification, while many competitors charge up to hundreds of dollars per provider per month just for intake alone.
HIPAA-Compliant Healthcare Automation Platform



See Your Admin Time Drop in Weeks
The impact is visible quickly: fewer manual checks, faster verification, and cleaner front-end data flowing into billing. Schedule a demo to see the automation in action, hear the voice AI, and understand how Fuse can reduce administrative load while improving cash flow.

FAQs
How does Fuse automate the front end of the revenue cycle?
Fuse connects patient intake, insurance verification, insurance payer calls and patient cost estimates into one automated workflow. Patients enter their insurance details during intake, Fuse verifies coverage at the CPT (procedure code) level by checking insurance payer portals and calling payers directly, then Fuse returns AI summaries of benefits and generates upfront cost estimates tied to specific procedures, all without staff rework. This end-to-end process eliminates the manual handoffs between intake, verification and billing that create errors and delays.
How does Fuse's voice AI handle insurance payer calls?
Fuse's voice AI handles insurance payer calls automatically, freeing staff from long hold times and repetitive conversations. The voice AI checks benefits and confirms coverage details so staff can focus on patients instead of administrative work.
Is Fuse's patient intake included at no additional cost?
Fuse's patient intake is available at no cost to clinics using Fuse's insurance verification. Many competitors charge up to hundreds of dollars per provider per month for intake alone. Fuse's HIPAA-compliant digital intake captures insurance details and required forms upfront, feeding directly into automated verification.
Does Fuse require new software or a platform switch?
Fuse fits into existing workflows with no new software to install and no platform switch required. After a short onboarding call, Fuse starts learning the practice's existing workflows and customizes the automation to minimize disruption to the team.
How does front-end revenue cycle automation prevent claim denials?
Incomplete patient intake, missing insurance details and rushed eligibility checks create bottlenecks that lead to claim denials downstream. Fuse automates these front-end processes so eligibility and benefit details are confirmed before services are delivered, producing cleaner data flowing into billing and fewer denied claims.
What results can practices expect from Fuse revenue cycle automation?
Fuse reduces manual insurance verification work and insurance payer phone time while producing cleaner front-end data flowing into billing. Practices using Fuse see fewer billing disputes, stronger collections from clearer upfront patient cost estimates and improved cash flow, especially for higher-cost services.

