
Know Exactly What's Covered Before the Appointment
Patients call your front desk with two questions: "Is this covered?" and "What will I owe?" Basic eligibility checks can't answer either. They confirm a patient has active insurance, not whether their plan covers the specific procedure you're about to perform or what the patient will actually pay.
Fuse provides insurance verification by CPT code. That means checking coverage for the exact procedures you plan to bill, confirming copays, coinsurance, deductible application, visit limits, and prior authorization requirements before services are rendered. Your staff gets the details they need. Your patients get real answers.

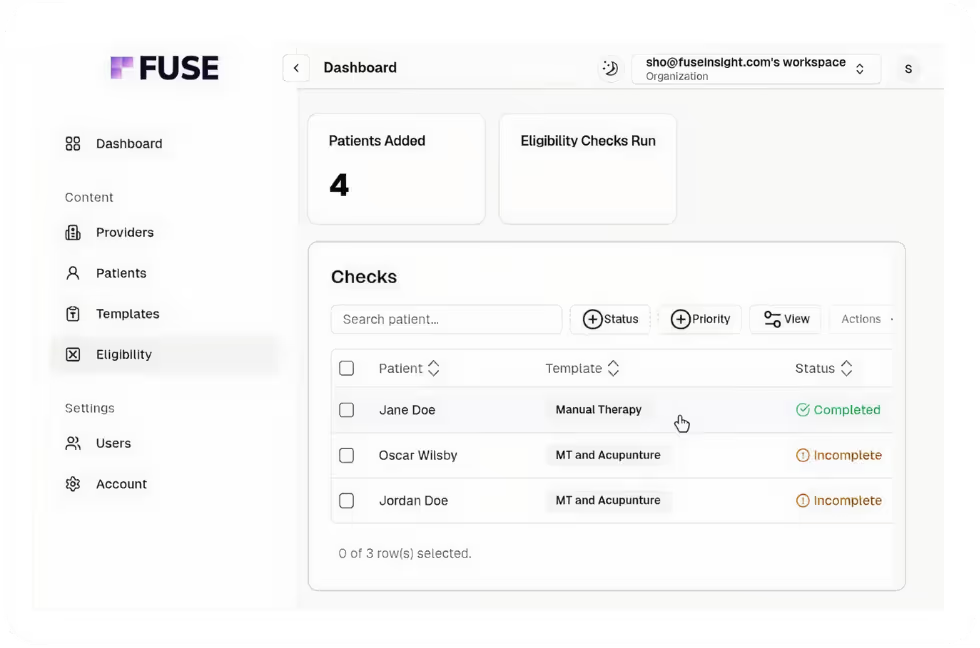








Why General Eligibility Checks Fall Short
Portals like Availity, pVerify, and Office Ally confirm that a patient has active coverage. They might show a specialist visit copay or a list of service type codes. But they won't tell you the exact copay for an initial psychiatric evaluation versus a follow-up therapy session, or whether a specific procedure code is covered at all. In many cases, they show multiple copay amounts without clarifying which one applies to your service.
That leaves your staff with three options: guess, call the payer and wait on hold, or bill and hope for the best. The result is predictable. Patients get surprise bills they weren't expecting. Your front desk fields calls asking why the charge doesn't match what they were told. Claims get denied for coverage issues that could have been caught before the appointment.
What CPT-Level
Verification Reveals
For each procedure code you plan to bill, Fuse runs a CPT benefits check to confirm whether the service is covered, the exact patient responsibility, and any requirements that could delay or deny the claim. This procedure-level insurance verification gives your staff what they need to answer coverage questions confidently at scheduling or check-in, not after the bill goes out.
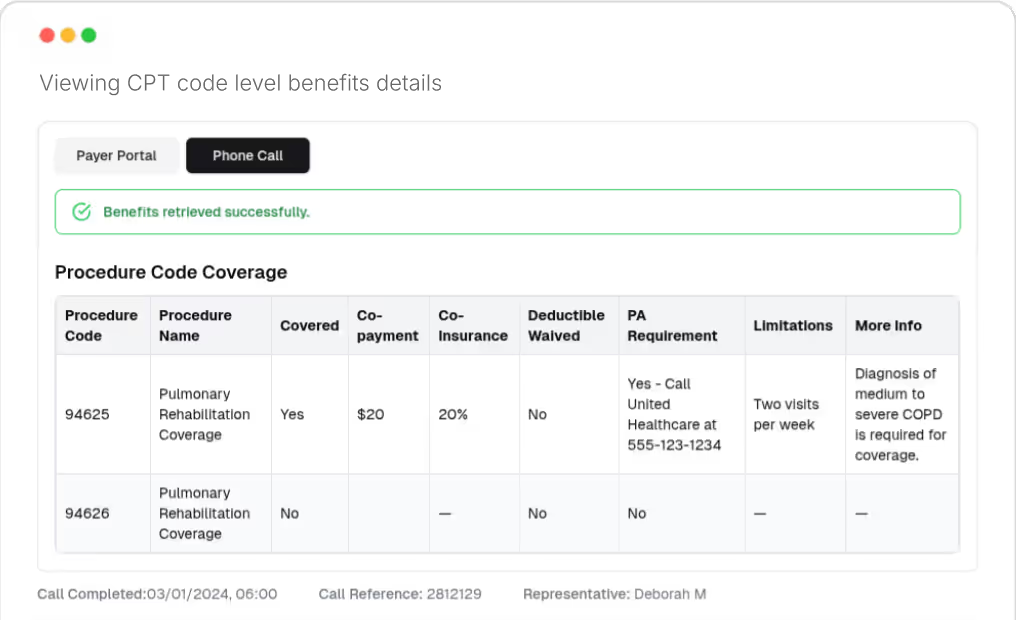
Coverage status (covered, not covered, or subject to limitations)
Exact copay amount for that specific procedure
Coinsurance percentage
Deductible application (does this service apply to the deductible?)
Visit limits
Prior authorization requirements
This level of detail answers the questions patients actually call about. When someone schedules an initial evaluation, your staff can tell them exactly what their plan covers and what they will owe. No callbacks, no guesswork, no "we'll let you know after we bill." Patients get real answers at the point of scheduling, and your team avoids the back-and-forth that eats up their day.
Payer portals rarely provide procedure-level benefits. To get that information, someone has to call the payer directly, navigate the phone tree, wait on hold, and ask the right questions. Fuse handles those calls automatically, pulling CPT-specific benefits data so your staff never has to pick up the phone or sit on hold for 20 minutes per patient.
Automated Portal Checks and Payer Calls
Portals provide baseline coverage data, but they rarely include procedure-specific details. The specifics, like whether a particular CPT code requires prior authorization, what the exact copay is, or how the payer classifies your billing provider, typically require a phone call. That is why CPT code level eligibility data is so hard to get at scale.
Fuse automates both. We check payer portals for general eligibility and then place direct payer calls to fill in the gaps. The results are combined into a single, clear summary. Your staff gets complete benefits information without toggling between portals, dialing payer lines, or reconciling conflicting data.
- Payer portal checks for baseline coverage data
- Direct payer phone calls for CPT-specific benefits
- In-network/out-of-network status confirmation


Accurate Estimates, Fewer Billing Calls
When you know the exact copay, coinsurance, and deductible for each procedure before the appointment, you can give patients a real cost estimate. Not a range, not a guess. An actual number based on their plan and the services you plan to bill.
Patients who know what they owe before they walk in do not call afterward asking why the bill is different. Your front desk spends less time on the phone explaining charges, and your billing team submits cleaner claims because coverage and authorization requirements were confirmed before services were rendered.
Fuse uses real-time insurance data and your specific CPT codes to generate fee estimates for your exact services. While final costs may depend on factors like the actual care received and claim processing, most estimates fall within a small margin of what patients pay. That gives both your practice and your patients the confidence to plan ahead.


Stop Fielding Coverage Questions
Every call from a patient asking "Is this covered?" or "What will I owe?" is a call that CPT-level verification prevents. When your staff can answer those questions at scheduling or check-in, patients get clarity upfront and your front desk gets time back.
Schedule a demo to see how Fuse automates CPT-level benefits verification through portal checks and payer calls, giving your team the coverage details they need without manual work.
FAQs
What is CPT-level benefits verification?
CPT-level verification checks insurance benefits for specific procedure codes rather than just confirming general eligibility. This reveals exact copays, coinsurance, and deductible amounts for each planned service, plus whether prior authorization is required and whether visit limits apply. Basic eligibility only confirms a patient has active coverage. CPT-level verification confirms what that coverage actually pays for specific procedures.
Why can't payer portals provide CPT-specific benefits?
Payer portals like Availity, pVerify, and Office Ally are designed for general eligibility checks, not procedure-level benefits. They typically show information like specialist visit copays or service type codes (STCs), but often cannot specify the exact copay for a particular CPT code or whether a specific procedure requires prior authorization. Getting CPT-level details usually requires direct payer phone calls.
How does Fuse automate payer phone calls?
Fuse uses AI to place direct calls to insurance payers, navigate their phone systems, and extract CPT-specific benefits data automatically. The system gathers coverage details, copays, coinsurance, deductibles, visit limits, and prior authorization requirements for each procedure code, then compiles results into a summary your staff can use immediately.
Can CPT-level verification identify prior authorization requirements?
Yes. Fuse identifies prior authorization requirements at the CPT code level during the verification process. Catching auth requirements before scheduling prevents denials from missing authorizations, one of the most common and avoidable reasons claims get rejected.
How accurate are patient cost estimates from CPT-level verification?
Patient cost estimates from CPT-level verification are significantly more accurate than those from general eligibility checks, with most estimates falling within a small margin of final patient responsibility. Fuse generates these estimates using real-time insurance data and your specific CPT codes. Exact costs may vary based on actual care received, claim processing, and any benefit changes at time of service.


